Neurofeedback for Mental Health Issues
Mental health issues are a drag
It is no fun to feel sad, mad, in pain, scared, nervous, spacy, foggy or desperate. Any one of these is bad enough. Combinations of these symptoms are even worse.
Moodiness, nervousness, fear, inattention, insomnia, migraine, addictions, and many other issues are irritating. And they are unnecessary with EEG biofeedback (neurofeedback). The remedy is in the root. In the physiology of the brain.
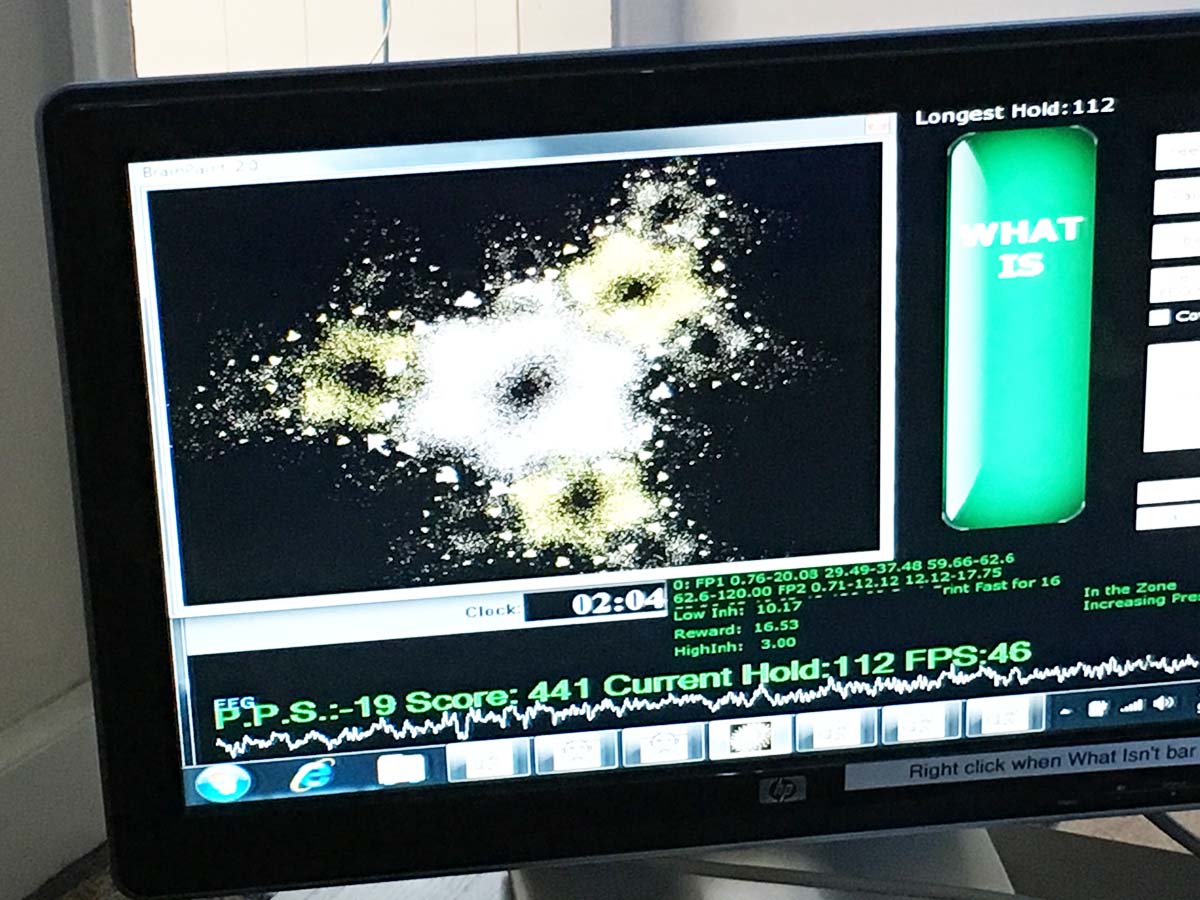
Psychological issues are linked to imbalances in brain waves. Too many or too few brain waves in the slow, medium or fast frequencies are bad habits that can be changed. In neurofeedback, I read your brain waves (neuro) and you are guided with computerized sounds and images (feedback) toward a balanced state. You practice becoming more sane during every session. Learning expands and lasts.
After training, most of my clients tell me they feel emotionally calmer and more mentally focused. They are much less burdened by their mental health issues. They report that their problems are either gone, reduced or are more manageable. They are able to proceed in their lives, achieve goals and enjoy new capabilities.

Gary Ames is a licensed psychologist specializing in Neurofeedback
This is not talk-oriented therapy. We will talk, but the main work is learning with the brain-computer interface. Neurofeedback is done without medication, invasion or side effects. You will learn to make better brain waves dozens of times per second. And the results last a lifetime.
Neurofeedback gives you a much better quality of life and effectively addresses the conditions outlined below. Just click on any condition for more details.
Gary Ames shows BrainPaint EEG Biofeedback
Overview of neurofeedback — 80 seconds.
Conditions
Anxiety & PTSD
Anxiety goes way down. Whether you feel nervous, bad arousal, or emotional reactivity – whether you feel your racing heart or you get tightness – you’ll experience less of all that.


Migraines
Migraines reduce significantly or may cease. Clients see a marked reduction in the frequency, intensity and duration of headache pain. Just less bothersome.
Addictions
Addictions to substances and destructive behaviors can finally be controlled. It is possible to build the capacity to free yourself and feel that you are enough, as is. When you’re able to self-soothe, you don’t need the other stuff. Call me at 610.668-3223.

Will Neurofeedback work for you?
I’m Gary Ames, a licensed psychologist with consistent and significant success for each of the conditions listed above. 80-95% of my clients average a 50% reduction in symptoms within 3 months. These results last.
Typically, my clients report feeling more calm and focused. Most say their sleep, mood and cognition have improved noticeably. I’m most proud that many of my clients are able to reduce or eliminate their psychiatric medications.
After learning and teaching biofeedback in university, I returned to neurofeedback in 2003 with intensity. I quickly absorbed the basics and nuances of advanced techniques. I have used a variety of neurotherapy systems and am delighted with the advanced tools I use now.
First, read about a condition that is dragging down your life. Then, when you are ready, either: make an appointment, send me a note, or call me at 610.668-3223.
I see clients from Montgomery, Delaware, Philadelphia, Chester, and Bucks counties and South Jersey.

Gary Ames is a licensed psychologist specializing in Neurofeedback
“I can’t believe how much this biofeedback helped me overcome that head trash.
Life is so much better now.”
“I used to have mental problems that would consume my life.
But now I’m just living a great life.”
“This is amazing. I feel so good every time we are done with a session.
Such a huge impact on my life. Thank you.”
“Biofeedback has been great for me.
It really worked to overcome my issues.”
“I have grown so much over the past 2 months.
This freedom is wonderful.”
“I used to have a slew of problems.
Those are gone now and I have moved on.”